Pat Summitt's Legacy: Insights and Reflections from Tyler Summitt

Pat Summitt was a legendary figure in women's basketball, renowned for her exceptional coaching career at the University of Tennessee. Born on June 14, 1952, Summitt became the head coach of the Lady Volunteers in 1974 and went on to achieve remarkable success over the next four decades. With an unparalleled commitment to excellence, she guided her teams to eight NCAA championships and notched an impressive 1,098 career wins, making her the winningest coach in NCAA Division I basketball history at the time of her retirement in 2012.
Beyond her coaching prowess, Summitt was admired for her leadership, integrity, and dedication to fostering the personal and athletic development of her players. Her impact on women's sports and her enduring legacy continue to inspire athletes and coaches alike. Summitt's indomitable spirit and contributions to the game have left an enduring mark on the world of basketball. Recently MDM Healthcare VP of Clinical Excellence Linda Robinson, MSN, RN, CPXP, was able to speak with Summit's son Tyler about her legacy, battle with Alzheimer's and her compelling story of resilience and generosity on our podcast PX Space.
The Pat Summitt Foundation, established in 2011 by Pat and Tyler Summitt, stands as a beacon of hope in the fight against Alzheimer's disease. The Foundation's mission, fueled by the founders' deep personal commitment, is to eliminate the heart-wrenching moment when families learn of an Alzheimer's diagnosis. Operating with a multifaceted approach, the Foundation channels its efforts into funding research for treatment and a cure, offering crucial care and support to patients and caregivers, and educating the public about Alzheimer's disease. Through strategic grants, the Foundation addresses vital components such as research advancement, disease awareness, and support services. Contributions to the Pat Summitt Foundation are managed by the East Tennessee Foundation, which plays a pivotal role in facilitating grants to organizations aligned with this noble mission.
"When Mom received her diagnosis, she expressed two powerful desires: to kick Alzheimer's to the curb and to take her 'Definite Dozen' principles out into the world, extending beyond sports into the realms of business and beyond. In response, Mom and I co-founded the Pat Summitt Foundation, and I established the Pat Summitt Leadership Group, dedicated to embodying her 'Definite Dozen' principles. Our diverse community, ranging from scientists to construction workers, restaurant staff to stay-at-home parents, engages in our online programs, listens to inspiring speakers, creating a truly impactful and inclusive environment,” said Tyler.

1. Respect Yourself and Others
2. Take Full Responsibility
3. Develop and Demonstrate Loyalty
4. Learn to Be a Great Communicator
5. Discipline Yourself So No One Else Has To
6. Make Hard Work Your Passion
7.Don't Just Work Hard, Work Smart
8. Put the Team Before Yourself
9. Make Winning an Attitude
10. Be a Competitor
11. Change Is a Must
12. Handle Success Like You Handle Failure
"In the videos and principles my mom shared, people continue to learn. Our Pat Summitt Leadership Group includes healthcare providers and a diverse mix of individuals in the online program, engaging with the Definite Dozen. Mom was passionate about this, and in a sense, it feels like we're carrying on her dream. We're actively working towards kicking Alzheimer's to the curb and assisting people in finding success, no matter their path in life. With the Pat Summitt Leadership Group, we're living out her vision,” said Tyler.
He further reflected on his mother’s legacy.
“It’s just so cool that people can still learn from her from her. They can still see videos, corporate speeches that she gave to large companies, we have those recorded and she's still teaching,” he said.
Pat and her son Tyler’s story demonstrates that in the face of devastating health diagnoses, patients and their families often exhibit remarkable strength, resilience, and a shared commitment to facing adversity with positivity and grace. The journey through a challenging health condition can be emotionally taxing, yet many individuals find solace and support in coming together as a united front. Through shared experiences, these families form bonds that transcend the boundaries of illness, creating a network of understanding and encouragement. Their collective positivity becomes a powerful force, offering hope, inspiration, and a testament to the human spirit's capacity to find light even in the darkest moments. In the Summitt’s story, the emphasis on grace and optimism not only aids in coping with the immediate challenges but also fosters a sense of empowerment and unity that proves instrumental in navigating the intricate landscape of healthcare with courage and dignity.
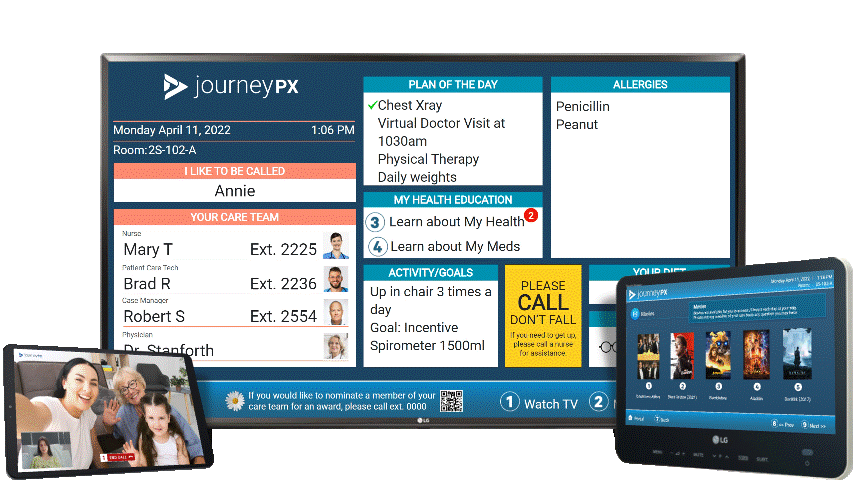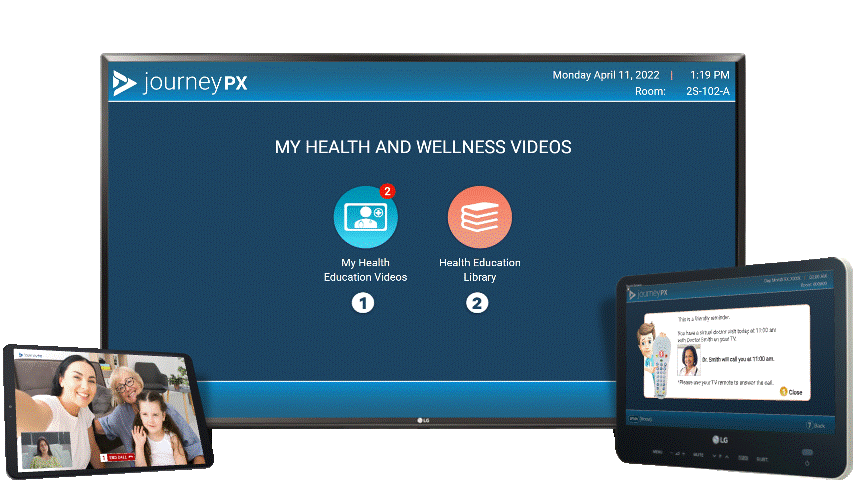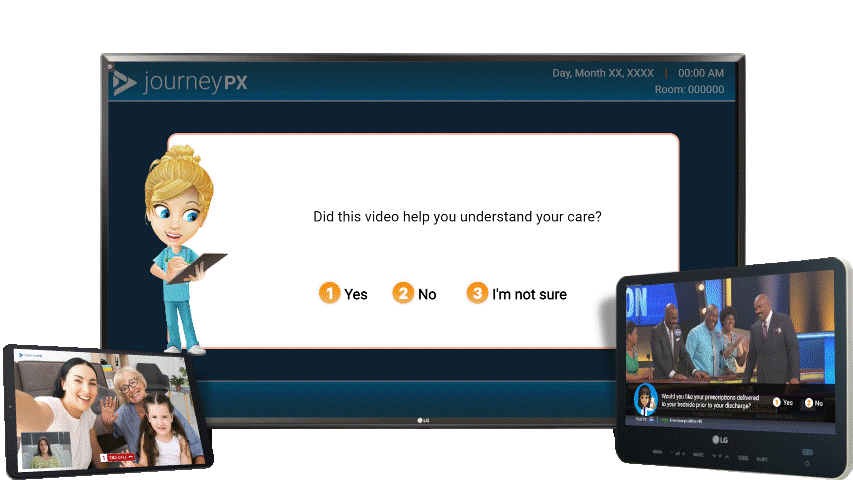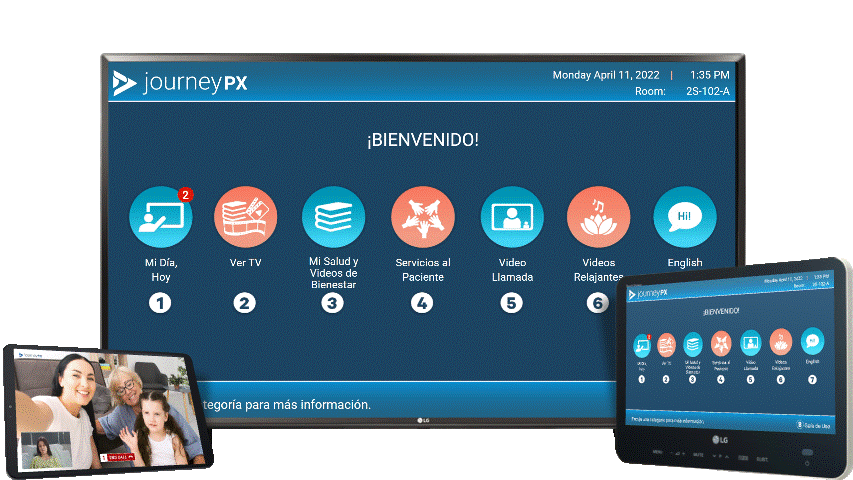
MDM Healthcare demonstrates a deep commitment to the well-being of patients and their families by prioritizing compassionate care and fostering a supportive environment. At the forefront of this dedication is the patient engagement platform Journey PX, a testament to MDM Healthcare's innovative approach. Journey PX goes beyond traditional healthcare services, offering patients and their families a range of tools designed to enhance their experience. Notably, the platform features a cutting-edge video solution, Connect, which facilitates meaningful connections between patients and their loved ones within hospital rooms. This unique feature provides a valuable opportunity for individuals undergoing medical treatment to connect with one another, fostering a sense of community and emotional support during challenging times. MDM Healthcare's dedication to incorporating such thoughtful and inclusive features into their patient engagement platform underscores their commitment to not only medical care but also the holistic well-being of those they serve.
For more information on the Pat Summit Foundation, visit patsummit.org. Additionally, to gain deeper insights into Tyler's reflections on his mother's legacy and their shared mission, listen to the full PX Space interview below.