By Ashton Elder and Linda Robinson, MSN, CPXP, RN, Vice President of Clinical Excellence, MDM Healthcare
In the current landscape post-pandemic, US hospitals find themselves grappling with formidable challenges. The pandemic has exacerbated an anticipated shortage of nursing labor and has placed added strain on an already fragile healthcare system. This strain bears the potential to adversely affect patient outcomes and amplify health disparities. At the core of the healthcare system, nurses are experiencing unparalleled stress, burnout, and uncertainties regarding their profession. In this context, it becomes imperative to explore avenues to enhance the healthcare system's functionality for the betterment of all.
Linda Robinson, MSN, RN, CPXP recently engaged in a conversation with Ramona Cheek, the Vice President of Nursing Transformation and Innovation at Bon Secours Mercy Health. Cheek introduces her pioneering research initiative, 'the way we work,' poised to reshape the entire care process, pledging enriched experiences for patients, nurses, and healthcare practitioners alike.
“We know that healthcare and nursing, especially the nursing workforce, have changed. We at Bon Secours Mercy Health have realized that the traditional approaches to staffing and organizing care delivery are not going to work in the future. So, the way we work initiative was born with the intent to reimagine care to provide care for the future,” she said.
This initiative seeks to reimagine the care process, ensuring enhanced experiences for patients, healthcare professionals, and all individuals engaged with hospitals. This innovative drive originates from Cheek's unwavering commitment to heed the voices of nurses who ardently expressed their longing for more quality time dedicated to patients.
“We started the initiative really simply and it was by going out and listening to the voices of nurses, and what we heard from the nurses resoundingly is that they want more time, they want more time to be with patients, to care for patients, to learn about caring for patients,” said Cheek.
The 'the way we work' initiative is fueled by the mission to recapture valuable time for nurses and is built upon four robust pillars, all underpinned by technology and digital solutions.
Cheek explains, “The way we work initiative is built on four pillars and a beam because I think the beam that supports all the other pillars, is, of course, technology and digital solutions. We know that in order for us to do things more efficiently and effectively, we are going to have to employ technology, we know that human resources are at a premium, and we are competing for that ever-shrinking pool of the best and the brightest for human resources. So, technology is going to have to be an enabler that really goes across our other pillars.”

Cheek highlighted the four foundational pillars underpinning this transformative initiative:
Revolutionary Care Delivery Models
The first pillar delves into revolutionary care delivery models.
"We must scrutinize diverse care delivery models and roles, asking ourselves which models will guide us into the future."
Streamlined Workflows and Communication
The second pillar encompasses streamlined workflows and communication.
"We recognize the necessity to reshape workflows and communication. We must shatter the barriers and comprehend our professional responsibilities, scope of care, and practice. This process will facilitate an environment of energy and synergy, allowing us to perform at the pinnacle of our training and education, delivering what our patients anticipate."
Support for New Nurses and Addressing Turnover
The third pillar centers on providing unwavering support for new nurses and addressing the pressing concern of swift nurse turnover.
"We are witnessing an influx of young professionals in the field, while experienced nurses are departing. We must ascertain how to furnish support to these newcomers."
Well-being of Nurses and Flexible Schedules
The fourth pillar concentrates on nurturing nurses' well-being, incorporating flexible work schedules to foster a healthier work-life balance.
"Our well-being holds significance, and achieving work-life integration is crucial. Our work environment must cater to these aspects."
It's vital to underscore that these pillars are all fortified by the beam of technology.
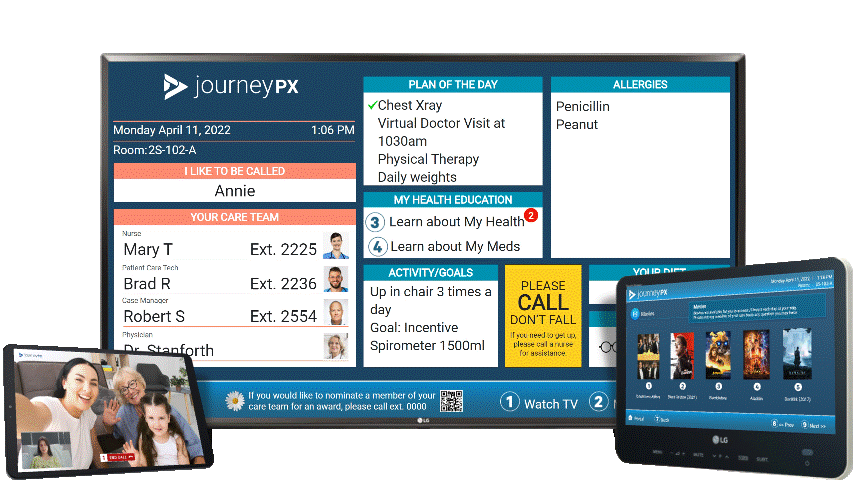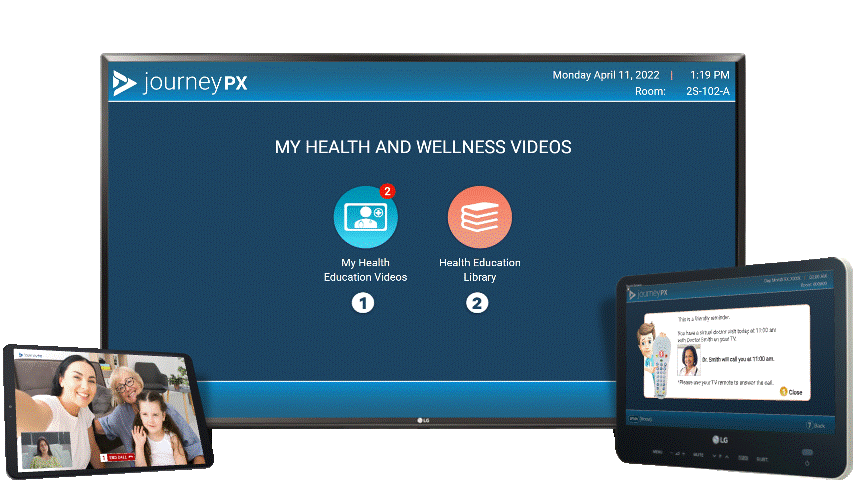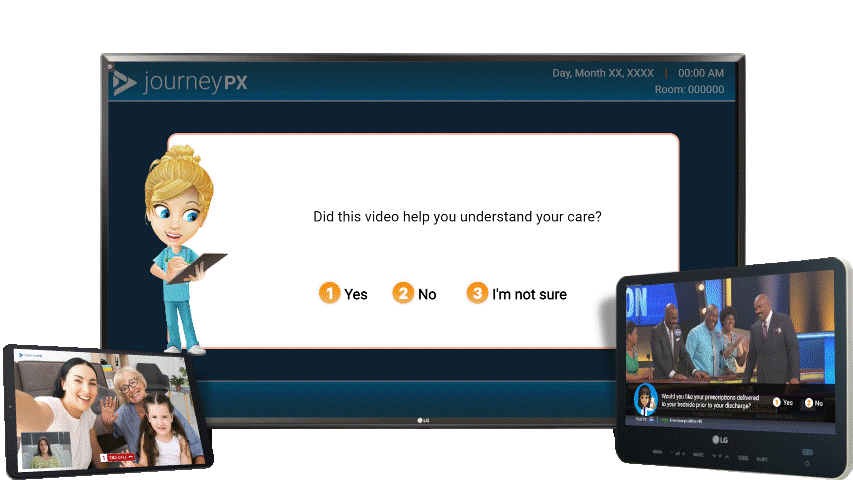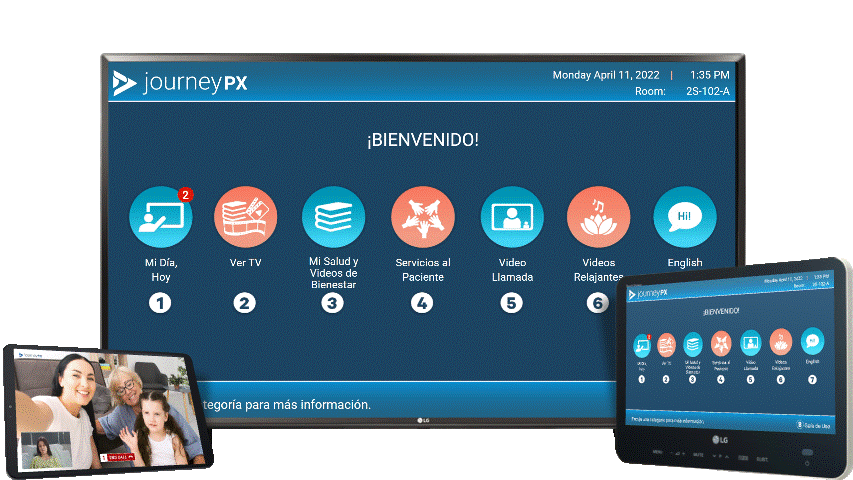
"Artificial intelligence in medicine and nursing will revolutionize our methods." This resonates with the transformative potential of technology in reshaping patient care. One such example is Journey PX, a state-of-the-art, cloud-based patient experience platform, heightening patient engagement throughout the care continuum. Journey PX aligns with all the pillars delineated by Cheek in the 'the way we work' initiative.
Optimizing Technology to Fit the Needs of Nurses
The conversation extends to the realm of virtual care. Cheek ponders, "Can a virtual nurse serve as an expert resource for new nurses in need of support?" This question reflects the innovative approach of utilizing virtual nursing to address the challenges posed by physical limitations.
Technology such as Journey PX Connect provides hospitals with the ability to bring additional experts to give that added layer of support. Journey PX’s Connect solution enables video calling for patients and families. The solution also provides a secure connection that allows for virtual visits and rounding by providers, nurses, other clinicians, and authorized staff. All of this is done through the patient’s TV in the room.
The interoperability of devices emerges as another significant consideration. Cheek elucidates, "Interoperability and stack ability are pivotal. Devices need to multitask, replacing individual devices addressing specific needs."
Journey PX solutions operate through the patient’s in-room TV. These solutions prepare patients for discharge by ensuring they remain informed about their daily care plans, receive tailored education, and streamline communication among patients, families, and care teams. The platform facilitates bedside shift reports, a cornerstone of quality and safety.

Time-in-Motion Study
Cheek's time-in-motion study reveals that time wastage by nurses predominantly occurs in medication and documentation tasks. Journey PX responds with tailored meds-to-beds programs, integrating with Electronic Medical Records (EMR) and engaging patients at the bedside to enhance medication health literacy. Additionally, Journey PX saves nurses valuable time when it comes to documentation as all of the information is updated in real-time and allows care teams to hardwire bedside shift reports and create LEAN clinical workflows.
Concluding her insights, Cheek offers a final reflection on the journey.
"The biggest realization is that these aren't challenges to solve, but dilemmas to manage."
She underscores the importance of nurses' voices and the trust they place in administrators to foster an environment conducive to patient care.
To delve deeper into Ramona Cheek's perspectives, you can listen to the complete PX Space podcast interview below.